Fluoroscopy-guided spine procedure
Lumbar Facet Radiofrequency Ablation
If your lower back pain is coming from the small joints in your spine — not from a pinched nerve — this is the procedure I reach for. It uses heat to quiet down the tiny nerves that carry the pain signal, and the relief usually lasts months to over a year.
What I'm doing
Turning down the volume on the pain signal
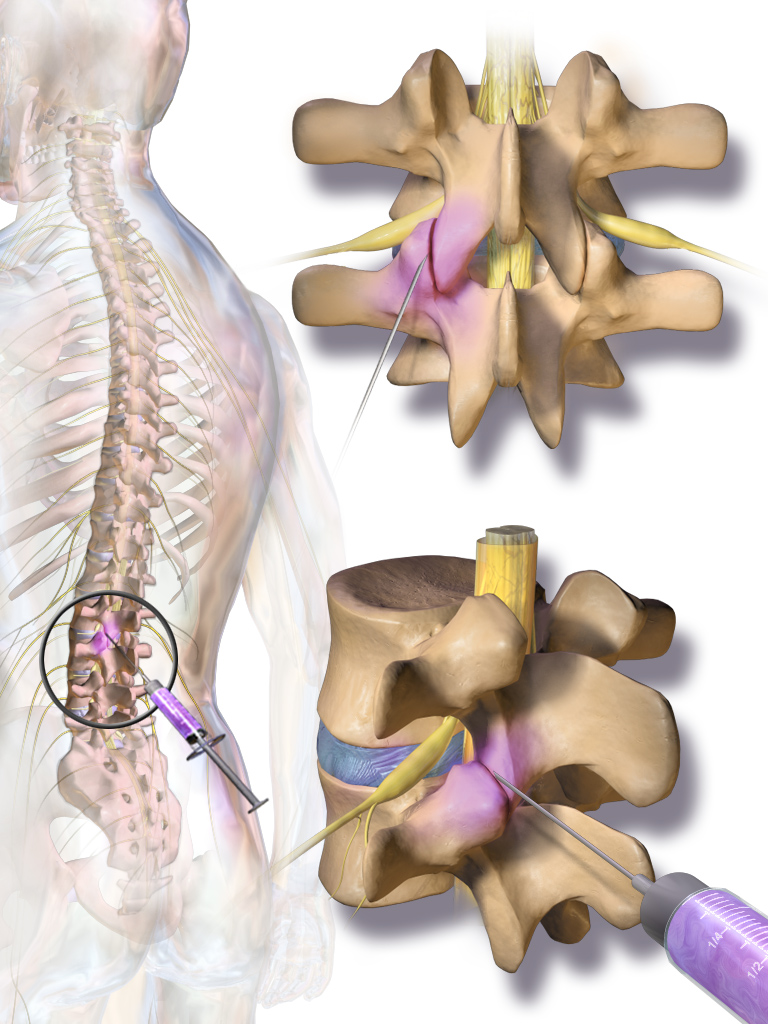
Your spine has small joints called facet joints — paired up at every level, like the hinges that let your spine bend and twist. When they wear down or get arthritic, they hurt. The pain signal travels through tiny nerves called medial branches.
Radiofrequency ablation uses controlled heat to interrupt those medial branch nerves. The joint stays. The arthritis stays. The pathway that carries the pain signal up to your brain is what changes. Patients describe it as someone finally turning down a radio that had been blasting all day.
Before I do an RFA, I almost always do diagnostic medial branch blocksfirst — usually two of them on separate days. I numb the same nerves with a temporary anesthetic. If the blocks give you significant relief while the medication is active, I know the facet joints are the source. If they don't, RFA isn't going to help, and we should look elsewhere. That two-step process protects you from going through a longer procedure that won't work.
I want to be straight with you about something: not everyone responds to RFA, even when the diagnostic blocks were positive. Most patients do — but a real fraction don't get the relief they'd hoped for. That's not failure on either of our parts. It's biology. We'll talk about what to do next if that happens.
Honest expectations
What this can do — and what it can't
Most patients who pass the diagnostic-block step get meaningful, lasting relief. But not every nerve responds the same way, and I want you to walk in with the right picture.
What this can do for you
- Long-lasting relief — typically 6 to 18 months from a single treatment.
- Often cuts or eliminates the need for daily pain medication.
- Lets you get back to walking, working, sleeping, and the things you've been missing.
- Minimally invasive — needles only, no incision, no stitches, same-day discharge.
- Repeatable. The nerve regenerates over time, and we can treat it again when it does.
Risks I'll be honest about
Most are manageable and short-lived.
- Soreness and muscle aching at the treatment sites for several days(common)
- Temporary numbness or skin sensitivity in the treated area(common, fades)
- A small percentage of patients don't get the expected relief(uncommon but real)
- Brief flare of your usual pain in the first week(occasional)
- Infection at the needle sites(rare)
- Nerve injury affecting movement (the medial branch is small and sensory only)(very rare)
Other options
Things we could try instead, or alongside
RFA is one of several reasonable paths. The right choice depends on what your pain actually is — and how much you've already tried.
Repeat facet joint injection
A direct steroid injection into the facet joint itself can give weeks to a few months of relief.
Where this fits: When you've responded well before and want a familiar, lower-commitment option.
Physical therapy and core stabilization
Strengthening the deep stabilizers of your spine often reduces facet joint loading and pain.
Where this fits: Always — usually as the long-term plan that an RFA gets you back to.
Epidural steroid injection
If your imaging or symptoms also suggest a pinched nerve, an epidural targets a different problem.
Where this fits: When pain shoots down a leg with numbness or tingling — that's nerve-root, not facet.
Anti-inflammatory medications
NSAIDs (ibuprofen, naproxen, meloxicam) can dial down facet joint inflammation.
Where this fits: First-line, especially during a flare, if your kidneys and stomach tolerate them.
Surgical consultation
If imaging shows instability, severe stenosis, or a structural problem that won't be fixed by quieting nerves, surgery may be the right move.
Where this fits: When conservative + interventional care has failed and the imaging clearly explains the symptoms.
Doing nothing yet
Sometimes the right call is to wait, optimize the basics — sleep, weight, posture, conditioning — and revisit.
Where this fits: Mild, intermittent pain without red flags.
Before your visit
How to get ready
A few important things — please read all of them. Skipping any one of these can mean we have to cancel and reschedule, which I'd rather not do.
One thing I want you to know first
You will not be put to sleep for this.A lot of patients walk in expecting general anesthesia — that's not what happens here. If we're using conscious sedation (only at the surgery center, only in select cases), you'll get a relaxant through an IV that takes the edge off. You'll still be awake. You'll still be able to talk to me. You just won't be anxious. Most patients say it felt easier than they imagined.
Bring a driver
Eating and drinking before
Take your morning medications
Blood thinners — talk to me first
- • Aspirin (81 mg) — usually OK to continue. I'll tell you if I want it held.
- • Plavix (clopidogrel) — typically held 5–7 days before
- • Eliquis (apixaban) — typically held 24–48 hours before
- • Xarelto (rivaroxaban) — typically held 24–48 hours before
- • Pradaxa (dabigatran) — typically held 24–72 hours, depending on kidney function
- • Warfarin (Coumadin) — typically held until INR is below 1.5
- • Lovenox (enoxaparin) — typically held 12–24 hours
Tell me about your allergies
What to wear
The day of
Step by step, what actually happens
The whole appointment runs about 1.5–2 hours. The procedure itself takes 30–45 minutes — longer than an epidural because I'm treating multiple nerves at multiple levels.
- 1
Arrival and check-in
You'll come in with your driver, finish paperwork, change into a gown, and a nurse will start an IV.
- 2
I see you before we start
I'll come in, go over the plan and which levels we're treating, answer questions, and confirm consent. Last chance to mention allergies, medications you're not sure about, or anything weighing on you.
- 3
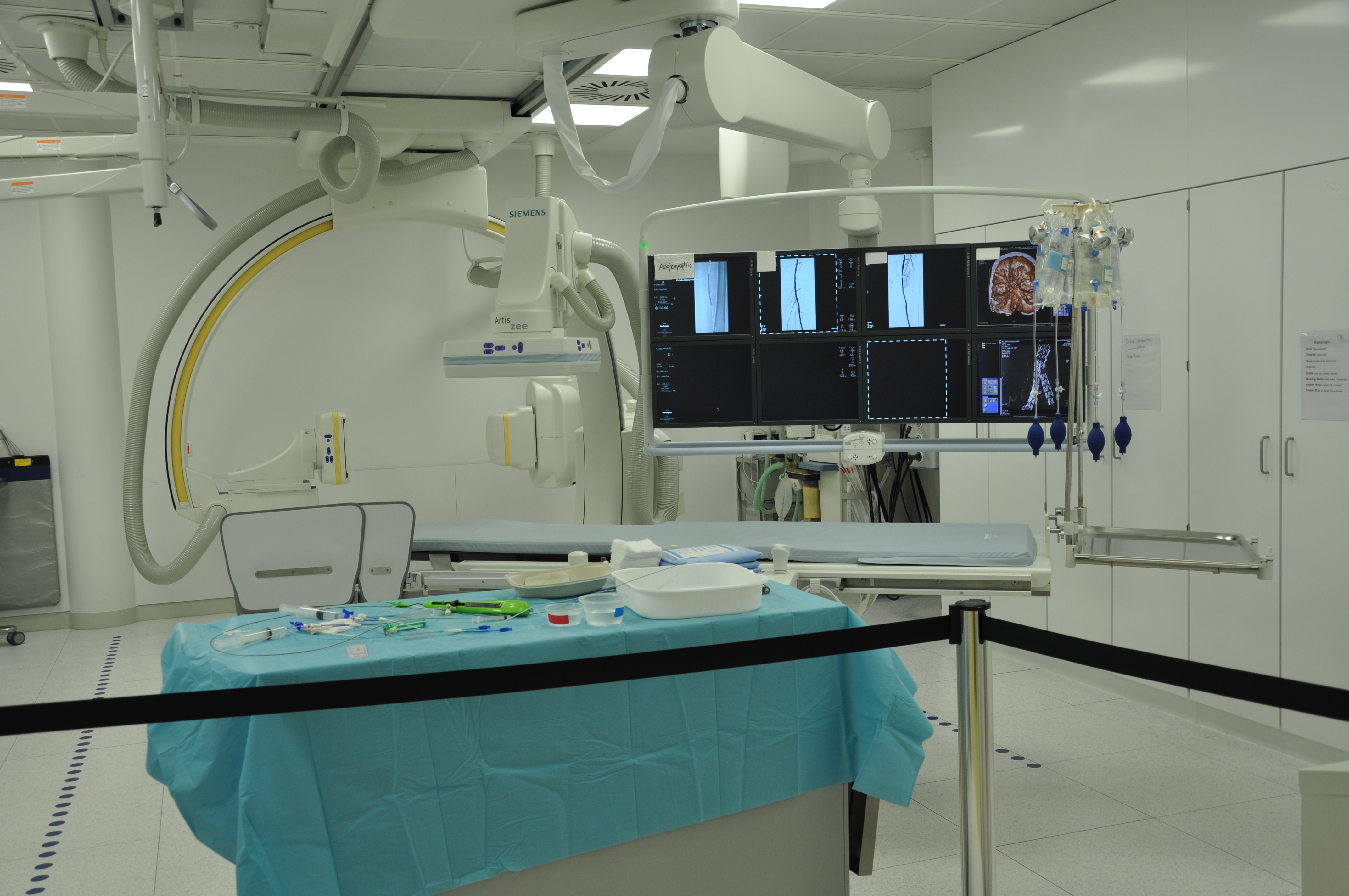
Into the procedure room
You'll lie face down on the procedure table. The C-arm X-ray sits over you, with a monitor beside it. Your back is cleaned with sterile solution and draped.
- 4
Numbing the skin
I'll inject local numbing medication into the skin and deeper tissue at each spot we're treating. You'll feel a few seconds of stinging, then it goes numb.
- 5
Positioning the probes
Using live X-ray, I guide thin RF probes to each medial branch nerve. I test each placement first with a brief electrical pulse — you may feel a familiar twinge at the joint or a tap in the muscle. That tells me I'm in exactly the right place.
- 6
The treatment itself
Once positioned, the probe heats the nerve to about 80°C for 60–90 seconds. You'll feel warmth, pressure, sometimes a deep ache. Most patients describe it as bearable. I treat the nerves on both sides at the targeted levels.
- 7
Recovery
About 30 minutes in recovery — vital signs, snack, walking around. Then your driver takes you home. You'll be sore.
After
The recovery you should plan for
The first week is the hardest part. Knowing that up front saves a lot of unnecessary worry on day three when your back is achy.
Days 1–5: the sore phase
Expect deep muscle achiness at the treatment sites — like a sunburn buried inside your back. Ice 15–20 minutes a few times a day. Tylenol or your usual pain medication for breakthrough discomfort. Light walking is fine; no heavy lifting.
Week 1–2: the transition
Soreness fades gradually. Your usual pain may still be present — this is the in-between window when the nerves haven't fully quieted yet. Don't judge the result here.
Weeks 2–4: real benefit shows up
This is when most patients notice the turning point. As the treated nerves stop firing pain signals, your back feels different. Resume normal activity. Start or restart physical therapy.
Months 1–18: sustained relief
Most patients enjoy 6 to 18 months of meaningful improvement. The nerves slowly regenerate over time, which is the design — and it means we can repeat the procedure when pain returns. Repeat RFAs usually work just as well as the first.
When to call me right away
Severe new weakness in your arms or legs
If a limb feels significantly weaker than before — trouble lifting it, dragging a foot, dropping things — that needs attention now.
Loss of bladder or bowel control
Sudden trouble holding it or sudden trouble going. Rare, but a true emergency. Go to the ER, then call me.
Fever above 101°F (38.3°C)
A fever in the days after the procedure, especially with chills, can mean infection.
Spreading redness, warmth, or drainage at the injection site
Some bruising and tenderness is normal. Pus, increasing redness expanding outward, or yellow drainage is not.
Severe new pain that's worse than before
Brief soreness for a few days is expected. Sharp, severe new pain different from your usual is not.
For anything that worries you, call my office. I'd much rather hear from you and tell you it's fine than have you wait at home wondering. For loss of bladder/bowel control or anything that feels like a true emergency, go to the nearest ER — then call me.
The questions I get most
Frequently asked
Will I be put to sleep?
Why do you do those nerve blocks before the RFA?
How quickly will I feel better?
How long does the relief last?
What if it doesn't work?
Can I drive myself home?
Will it hurt?
Can I have RFA more than once?
Have Questions?
If you'd like to learn more about your treatment options or have a question for Dr. Patibanda, reach out.
Contact Dr. Patibanda